Lymphedema Risk and Massage Therapy or Esthetic Care
A Few Lymphedema Basics
Lymphedema is a condition that can occur at any time after cancer treatment, even many years later. It impairs normal drainage of fluid through the lymphatic system, causing swelling. American lymphedema educator, Joachim Zuther, defines lymphedema as “protein-rich edema.” The backed-up fluid contains not only the watery component but also excess protein, bacteria, virus, and cellular debris.
Certain cancer treatments can create a disruption in the lymphatic system, which puts a person at risk for developing lymphedema months to years afterwards. The most common causes are radiation to or surgical removal of lymph nodes from the neck, armpit, or groin. The combination of surgery and radiation increases the risk. There are no solid statistics indicating how many patients develop lymphedema. The numbers range from as low as 5% to as a high as 55%.
-
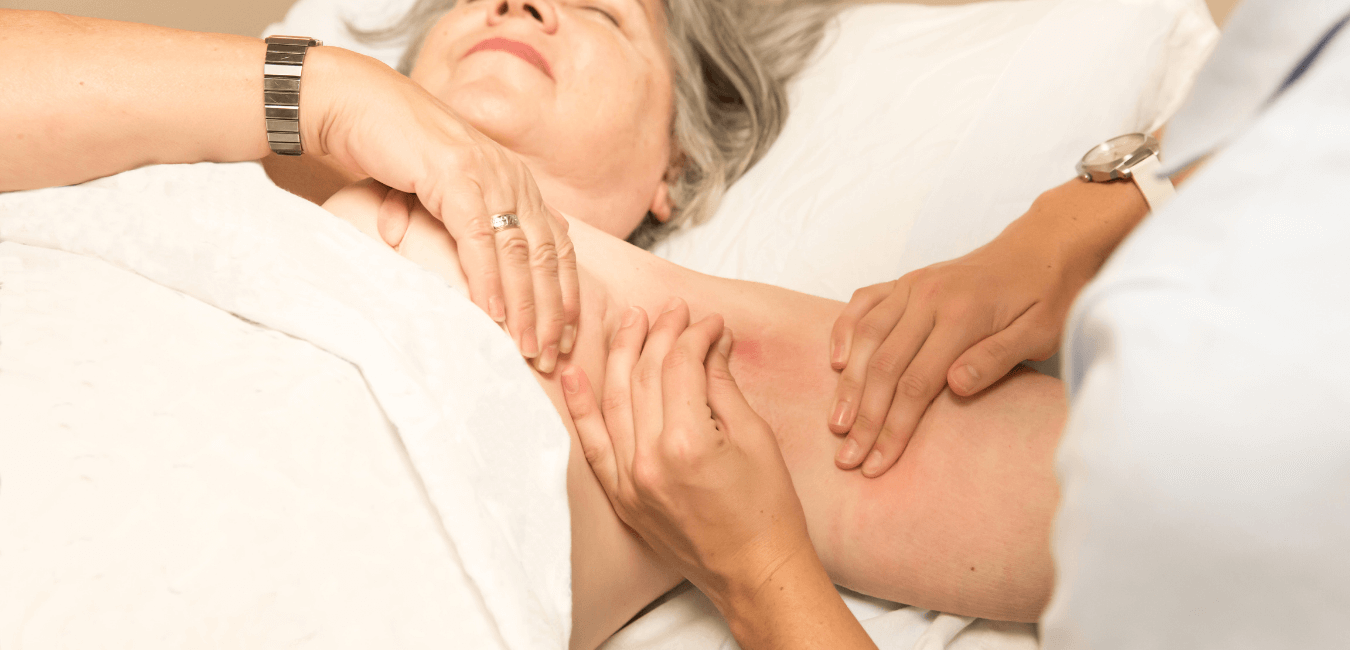
The main tenet of oncology massage and oncology esthetics is adaptation. Lymphedema, or the risk of it, is one of the common side effects requiring adaptation. There are guidelines that help therapists design a treatment plan for those who are at risk for or who have lymphedema. The goal is to provide massage or esthetic care that safely includes the affected areas without triggering swelling or exacerbating it. The main adjustment is to the amount of pressure. Additionally, the direction of strokes in the affected areas should follow a certain pattern to support flow of the lymphatic system.
Oncology massage therapists and estheticians are trained to provide a safe supportive session, not to manage lymphedema. These therapies tend to work with the musculoskeletal, integumentary (skin), and the nervous systems. They are not designed to address the lymphatic system specifically, although both may influence this system either positively or negatively. It is vitally important to seek massage from a qualified oncology massage therapist even years after treatment is completed. A massage therapist or esthetician who is unaware of these precautions may unintentionally trigger or exacerbate swelling.
-
Learning the modalities to treat lymphedema is a process requiring weeks to months. Physical and occupational therapists are often trained in these disciplines. Some massage therapists, however, have gone to the lengths required to complete these trainings and can provide lymphedema management. Often, they work in conjunction with the physical or occupational therapist during the rehabilitative and management phase of lymphedema care.
The most commonly known lymphatic management techniques are Complete Decongestive Therapy, Manual Lymph Drainage, Lymph Drainage Therapy, or Complex Lymphatic Therapy. All of these techniques have the same ultimate goal, moving the excess fluid toward lymph nodes that are undamaged and have open pathways.
At this time there is no cure for lymphedema. However, lymphedema techniques can reduce the amount of swelling and improve tissue quality. The result is increased comfort, mobility, and quality of life.
-
The warning signs of lymphedema may include the following symptoms in the areas of and around where you were treated for cancer:
- Heavy or achy feeling
- Tightness or decreased flexibility in the joints and surrounding tissues
- Slight pitting at the sites of rings, bracelets, or elasticized clothing
- Noticeable swelling
- Pain, numbness or tingling
-
Edema is usually caused by excess tissue fluid that had not yet returned to the circulatory system.
Lymphedema is swelling caused by excess protein-rich lymph trapped within the tissues.
-
- Academy of Lymphatic Studies
- Brennan School of Innovative Lymphatic Studies
- Casley Smith International
- Chikly Health Institute
- Foeldi College
- International Lymphedema & Wound Training Institute
- Klose Training
- LeDuc Training
- Norton School of Lymphatic Therapy
- Pacific Therapy Education, Inc.
- Vodder School International
To learn more about lymphedema
Visit the LE&RN (Lymphedema Education and Resource Network) website